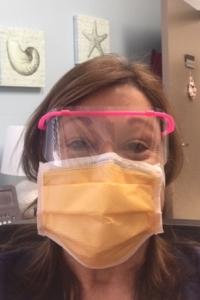
"Am I worried about becoming one of the positive? Absolutely!" Lynn Wiles said. "... I'll protect myself as best as I can - but I do worry."
By Irvin B. Harrell
Every semester, faculty at Old Dominion University's College of Health Sciences pour their hearts into preparing the next health-care providers. Many are young, innocent souls who still have so much to learn about selflessly dedicating their lives to save others and inevitably will devote themselves "to the welfare of those committed to their care," in the words of Florence Nightingale, the founder of modern nursing.
At the same time, these instructors work double-time in the field, fulfilling the same pledge. Many of these professionals now find themselves on the front lines of a pandemic that is wreaking havoc on our global population with no real end in sight. COVID-19 has changed education at ODU. It has transformed the lives of many of instructors, who have been called into action and flinch not in the face of adversity and possible infection.
ODU faculty members Lynn Wiles, Beth Tremblay and Donna Rose are but three of these health-care professionals. Their stories offer a passionate prism through which to view their efforts to support their students, help others, battle an unseen enemy, prepare for the unknown and find balance and some sense of normalcy in their own lives.
Wiles, a staff nurse at Sentara Virginia Beach General Hospital's emergency department, has been working in the emergency field longer than she has been teaching. She chose to stay in that front-line setting not only for her love for bedside nursing, but also because of the ways it informs her classroom instruction.
"I think it's critical to remain current with clinical practice given that I teach didactic and clinical courses that are acute care and patient-focused," she said. "I also love being a resource for the staff and students and enjoy working with my clinical team members to develop evidence-based practice projects and staff education."
While COVID-19 has produced its unique set of problems and fears of exposure, emergency departments are environments where exposure to diseases are a constant concern. Working in them can mean susceptibility to a host of pathogens, including HIV, hepatitis and influenza, Wiles said. That's why personal protection equipment (PPE) has become increasingly important.
"I started patient care before the Centers for Disease Control and Prevention (CDC) guidelines for standard precautions and routine glove use," she said. "Am I worried about becoming one of the positive? Absolutely! ... I'll protect myself as best as I can - but I do worry."
Since the COVID-19 pandemic, Wiles' life has transformed into a dizzying juggling act. Balancing her work among ODU, the emergency department and the home has been challenging. She no longer leaves the house (other than walks or bike rides) except to go to the hospital on Thursdays. Her family does the grocery shopping because of her higher risk to exposing others. She hasn't seen her mother in weeks.
"I've turned my master bedroom into my quarantine spot if needed, including a working area," she said. "Right now, I still hang out with my family, but definitely at a great distance. We are using lots of Facetime and Zoom to communicate."
Wiles' ODU schedule is "Zoom-packed," consisting of 8 a.m. to 5 p.m. most days, she said. Her husband Chris works the same hours from his home work space as an IT systems analyst for Operation Smile, and her daughter Courtney, a sophomore at James Madison University, has her own study space as well at their home in Virginia Beach.
A beeping smart watch reminds Wiles when she hasn't been active enough while she is hunkered down in front of her computer. She responds by taking a break and going for a short walk. Come 5:30 p.m., her family finishes work and takes walks or goes biking as a distancing unit.
While her emergency room hasn't been overrun with patients, Wiles said she and her co-workers stay prepared in case of an onslaught of COVID-19 cases. But stress has taken a toll. Many co-workers have sent their children elsewhere because of the exposure risks.
"Remember, ER nurses tend to hook up with other first responders such as EMS, fire, police, all of which have horrible exposure risks and crazy schedules," she said. "Several also are juggling spouse deployment."
Through it all, the spirit of community has been the glue holding everyone together and easing anxieties, Wiles said.
"Health-care workers are banding together and stepping up for extra shifts. We are trying to protect each other," she said. "We are acknowledging everyone - not just those of us who provide care but the people not on the front lines who are cleaning, cooking, delivering supplies, etc. We are a team. And on the home front, families are taking time to be together. That's huge."
"The efforts from everyone to stay home so that we at the hospital don't become overrun with more patients that we can treat has been touching," Beth Tremblay said. "Nurses are always here for the community. It has been beautiful to see the community be here for us."
When Tremblay isn't lecturing at the School of Nursing, the Williamsburg resident works as a registered nurse in the intensive care unit (ICU) at Sentara Williamsburg Regional Medical Center. She has spent 25 years as a nurse, and has been in the ICU for about 13 years.
"What I quickly discovered is that I love the education and advocacy aspects of nursing," she said. "Those motivators have not changed for me and have guided my career. I was interested in the ICU because of the intensity and variety of cases, but also for the opportunity to work with patients and families at a time when they are most vulnerable."
Observing proper protocols for PPE and hygiene are key during viral outbreaks, Tremblay said, emphasizing that her concerns are more for her family and patients. She said she has "always had a ritual of sorts" for not "tracking in" unknown infectious agents at home.
Tremblay said her life has encountered disruptions during this pandemic, but they have been far from catastrophic. She counts herself fortunate to work at ODU given its quick conversion to online courses that have allowed her to work from her home. She goes to the hospital as needed to support regular staffing. And since all elective surgeries have been canceled, it has freed staff to help with other hospital units.
As for her students, Tremblay said she has had to boost her support for them - especially those struggling with illness in the family or having difficulty managing because they have children at home full time or increased work hours. She has to account for her own school work as well. She is working on a dissertation on vaping use, and the crisis has interrupted her data collection.
Working 12- to 13-hour shifts can be grueling, so Tremblay "typically takes a late start each day to give herself time to decompress and process."
"Decompression for me looks like getting outside for a walk with my dogs, working in my vegetable garden, or my home yoga practice," she said.
Tremblay's experiences during this crisis have been filled with positive moments, she said. Her hospital has been proactive in thinking ahead for innovative staffing solutions that will best care for the community. Her crew at the ICU has stayed positive and caring, with open and honest communication. Family and friends have chipped in to provide PPE to help lessen any shortages. Community cooperation, too, has been heartwarming.
"The community at large has been incredibly kind and grateful. We have rainbows drawn by children put up in our windows with words of gratitude," she said. "The efforts from everyone to stay home so that we at the hospital don't become overrun with more patients that we can treat has been touching. Nurses are always here for the community. It has been beautiful to see the community be here for us."
Tremblay notes one noticeable negative impact of COVID-19 in the ICU: the absence of family members at the bedside. Providing care for patients and helping them to connect the loved ones has taken on "an added dimension now," she said.
"Calling a husband or wife of my patient after an emergent intubation ... I know that they cannot come to the bedside for me to show them firsthand how I am caring for their spouse," she said. "What's more, I know that in most cases the patient is isolated. So, I really have to be cognizant to check in with them more often and also to help them develop a support plan for themselves. Even if they are physically alone, they need to have family and friends who will, figuratively speaking, walk through the storm with them."
"When I get home, my family makes sure I remove my scrubs and go straight to the shower before I touch or sit on anything," Donna Rose said.
Rose, a clinical assistant professor in the School of Nursing, is also an employee health registered nurse at Sentara Leigh Hospital in Norfolk. Rose touts the fact the she and her two daughters, Brittney and Ashley, are ODU graduates.
Working in employee health services has been a stark change from her 34 years as a bedside nurse, she said. Now her "patients" are her employees. Her job is to make sure employees are fit and safe to do their jobs. She assesses and evaluates. She facilitates annual health screenings, evaluates injuries and exposures, provides fit testing for N95 masks and determines whether employees are safe to return to work after absences for a variety of reasons.
"Ensuring that employees are up to date on vaccinations is a large part of the job also," she said. "I had no idea there would be so much to learn."
Exposure issues are not as high for Rose as they are for health-care professionals on the front line. However, she does wear PPE as a precaution. As for her full-time role at ODU, she works from home. She typically spends one day a week at the employee health office, but as of late, things have been busier and she has responded with picking up additional on-call shifts.
"When I get home, my family makes sure I remove my scrubs and go straight to the shower before I touch or sit on anything," she said.
Rose, like Wiles and Tremblay, teleworks at ODU. Her husband works at Norfolk Naval Shipyard, and her oldest daughter, Brittney, just completed her Ph.D. at ODU and is at home waiting to move to South Carolina to start a job.
Having a good team that works hard and still takes time to share occasional laughs has had a big impact on keeping up spirits at the hospital, Rose said.
"As you can imagine, our department has been very busy during this global health crisis," she said. "We have received so much support from our managers, from first-line team coordinators all the way up. They are constantly keeping us up to date, encouraging us and thanking us."
When asked about taking breaks or decompressing, Rose admits that she may not have the best habits given her profession.
"Unfortunately, nurses - as well as most health-care providers - do not care for themselves like they should. We become so accustomed ... to just doing what needs to be done and caring for patients, so I'm not exactly sure what a break looks like," she said. "With the travel restrictions and social distancing guidelines, I have tried to have more down time, when not working at one of the two jobs. I am doing more reading, walking and bike riding. And OK, maybe some Netflix binging and eating."
Wiles, Tremblay and Rose are a few of the many cogs in the nation's health-care system. Their roles in the current crisis are important to their communities that at a moment's notice could find themselves embroiled in an upsurge in COVID-19 cases. Equally important to these health-care professionals are the students that they equip for the future through the education they provide, their adherence to best practices and their inspiration. The three leave these parting words for students who feel the calling to one day put themselves on the front lines of a health crisis:
"Protect yourself," Wiles said. "Your passion to help is amazing, but we are not invincible!"
"Anyone who wants to be a part of this amazing 'club' will need to develop the ability to think through complex situations, emotional resilience and deep compassion," Tremblay said. "If you are up for the task, we welcome you with open arms."
"Although it may seem exciting at times like this, you must keep yourself as safe as you can while providing care to the patients," Rose said. "I would also say that we need you! If nursing is your calling then don't let this stop you."
Related News Stories
ODU Responds to Governor's Call for 30,000 Volunteers
How you can join the Virginia Medical Reserve Corps to support the community during the COVID-19 public health crisis. (More)
ODU’s College of Health Sciences, Hospital Connected Beyond Crisis
Lake Taylor Transitional Care Hospital in Norfolk is the beneficiary of donations of much-needed personal procective equipment. (More)
ODU Faculty and Students Answer the Call for Personal Protection Equipment
They’re helping to fill a critical need at local hospitals. (More)